Young physicians leaving public hospitals for private aesthetic clinics
Many residents prefer to move directly into private aesthetic medicine, which is more profitable and less risky. Known as “chokubi”, this phenomenon reflects difficulties and lack of investment in the public healthcare system, which risks matching South Korea's staffing shortages.
Tokyo (AsiaNews) – A growing number of young Japanese physicians are abandoning their main clinical specialities to move towards private aesthetic medicine, which is more profitable and less risky, this according to Dr Tomoaki Takei, a physician writing in Asia Sentinel.
The phenomenon he describes also affects South Korea, whose healthcare system has long been struggling due to a shortage of residents, especially in rural hospitals.
Getting a medical licence in Japan requires a long and demanding residency in public hospitals, which is why more and more recent graduates are choosing to invest the first part of their studies in the private sector, moving directly to aesthetic clinics after the mandatory two-year residency.
In Japanese, this practice is called Chokubi, which means "direct access to aesthetics”.
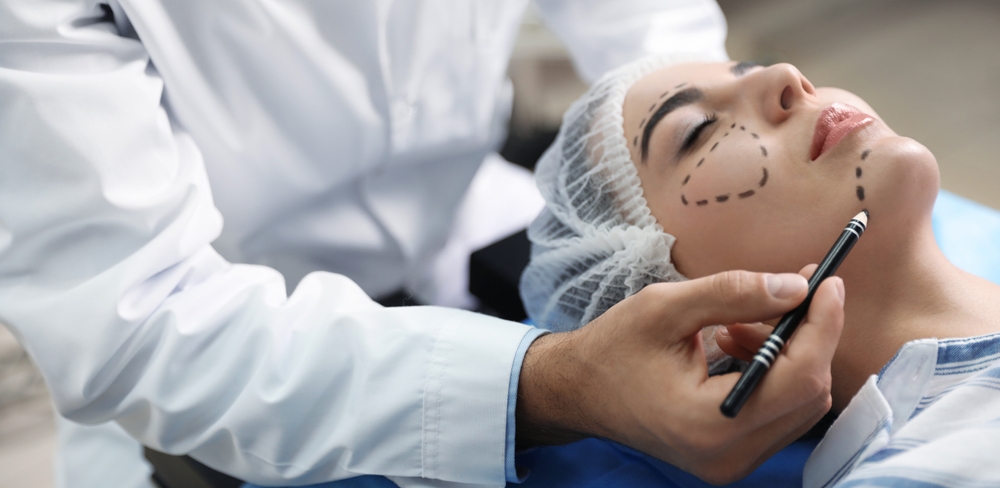
The clinics are unregulated private facilities, specialising in non-surgical or minimally invasive treatments – like Botox, dermal fillers, laser treatments, and chemical peels – that are highly sought after in Japan, where the demand for aesthetic procedures is rapidly growing.
Along with South Korea, Japan ranks among the world's leading providers of these types of procedures, which people value for their natural and minimally invasive results, especially among younger people.
According to some estimates, out of approximately 9,000 new professionals entering the healthcare system, more than 300 young doctors choose aesthetic clinics each year.
A seemingly limited loss, but one that over time risks emptying key specialities such as surgery, emergency medicine, paediatrics, and internal medicine, which are less profitable and increasingly less attractive fields due to the intense pressure doctors are subjected to.
This migration is driven by economic and cultural factors. Young Japanese professionals rely on two criteria to make the best choice for their future: cos-pa (cost performance) and tai-pa (time performance).
The traditional hospital career, with gruelling shifts, high legal responsibilities, and limited salaries, offers little return when considering either criterion.
By contrast, aesthetic medicine offers twice the starting salary of a university hospital surgeon, regular hours, and significantly lower legal risks.
The problem, Dr Takei notes, is structural because the Japanese healthcare system is based on a national public insurance system, which caps salaries for essential medical service providers, while the aesthetics sector, regulated by the private market, allows for much higher earnings.
In this context, the choice by young doctors appears less like a moral failing and more like a response to the distorted incentives of the healthcare system.
The same trend has been reported in South Korea, where the flight from essential specialities contributed to a health crisis that culminated in large-scale strikes in 2024.
There too, many physicians turned to so-called GP-Skin aesthetic medicine, attracted by better financial and working conditions.
In Japan, the same trend raises questions about the use of public resources. Medical training is heavily subsidised by the state, but when graduates move to the private sector, the return on public investment diminishes.
Furthermore, the shortage of doctors in hospitals risks compromising the transmission of skills between generations, weakening the system's ability to provide complex care in the long term.
Reforms are needed to address this problem, reducing inequalities between the public and private sectors: from increased compensation for key specialities and reduced legal risks to greater regulation of the aesthetics sector.
Proposals also include the introduction of a mandatory minimum period of service in hospital specialities before entering private practice, as well as potential mechanisms for redistributing resources.






.png)










